RANGOON — It was New Year’s Eve, 1996, but Ko Kyaw Thu was in high spirits for other reasons; he was being released after serving a three-year sentence at a prison labor camp near Bago.
“I had many dreams of what I would do after my release,” Ko Kyaw Thu, who is now in his late 40s, with a bronzed complexion and hair scraped back in a ponytail, told The Irrawaddy.
Ko Kyaw Thu’s dreams vanished at the blare of a car horn outside his house two days after his release. Four of his friends were inviting him to come out.
“We went to a teashop for a chat,” he recalls. “After a while, they said they were going to buy drugs and asked me to go with them.”
Detaching himself from his friends would be too difficult, he says, despite the fact they offered him drugs— the very substances that got him imprisoned three years earlier. He didn’t want them to think their relationship had changed.
They bought heroin and went to his friend’s house to take it.
“I refused to do it at first but my friends convinced me that one time wouldn’t make me addicted,” Ko Kyaw Thu says. “I snorted it, believing that as long as I knew how to avoid getting arrested, I could continue doing drugs.”
But that one relapse was enough for Ko Kyaw Thu to become hooked again. He was arrested in June the following year for illegal drug use — the same charge as before, and spent another three years in jail before being released again in 2000.
One of The Harshest Drug Policies
According to records obtained by The Irrawaddy from the Home Affairs Ministry’s drug enforcement department, 49,072 people were arrested on drug related charges between 2011-16, with an increase of 4,403 arrests from 2015 to 2016.
Citing these figures, Police Col Zaw Lin Tun, head of the Central Committee for Drug Abuse Control’s (CCDAC) project department, told The Irrawaddy that punishing drug users has not alleviated the country’s drug problem.
“Since the problem has not shrunk, we have come to realize that our policies are not the right approach,” he said.
Burma’s existing 1993 Narcotic Drugs and Psychotropic Substances Law prohibits anyone from planting poppy, coca, cannabis or any kind of plant from which drugs are derivable or extractable. It also criminalizes possession and use of any drug that the ministry declares to be a narcotic or psychotropic substance as well as substances containing such drugs.
The law aims to prevent the danger of narcotic drugs and psychotropic substances, “which can cause degeneration of mankind, as a national responsibility,” and to implement the provisions of the 1988 United Nations Convention Against Illicit Traffic in Narcotic Drugs and Psychotropic Substances.
It requires drug users to undergo treatment at government-recognized medical centers; failure to do so can mean three to five years in jail. Those found guilty of cultivating illegal plants or possession, transportation, or distribution of illicit drugs can be imprisoned from five to 10 years.
If the defendant is found guilty of any of these offenses along with the intent to sell the drugs, the sentence is a minimum of 10 years.
The Drug Policy Advocacy Group Myanmar said in its report in February that “there is no correlation between the severity or the intensity of law enforcement and the prevalence of drug use” according to several studies conducted around the world. The report also claimed that Burma’s drug law remains “one of the harshest drug policies” in the world.
To tackle Burma’s epidemic of illegal drugs, Col Zaw Lin Tun said draft legislation modifying the country’s notorious 1993 narcotics law would soon be submitted to Parliament.
“It would order an effective treatment policy for drug users rather than prescribe punishment and imprisonment,” he said.
Published on Mar. 17 and 18, the draft amendments would exempt drug users who are first-time offenders from imprisonment, instead referring them for treatment at a government medical center. According to the draft, second time offenders would have to sign a letter of intent at a court to seek treatment and third time offenders would be sent to rehab centers for three to five months.
Those who violate directives from the rehab centers would be assigned to do community service, which includes cleaning and repairing public places, with a minimum of 180 hours in total, two hours per day.
An Abundance of Drugs
Ko Ngwe Soe, who lives in Shan State’s Nyaung Shwe Township, told The Irrawaddy that his town had become flooded with methamphetamines pills, to the point where he wanted his teenage son to leave town after high school to avoid the fate of other young addicts.
“He can do anything he wants, but not drugs,” he said.
Each tablet costs 2,000 kyats, says Ko Ngwe Soe, the same price as a bottle of beer or a movie theater ticket.
Opium and heroin addiction has become widespread in Kachin, Shan, Chin and Karenni states, where there are sprawling opium plantations, as well as in transport hubs and border towns such as Lashio, Muse, Kalay and Tamu.
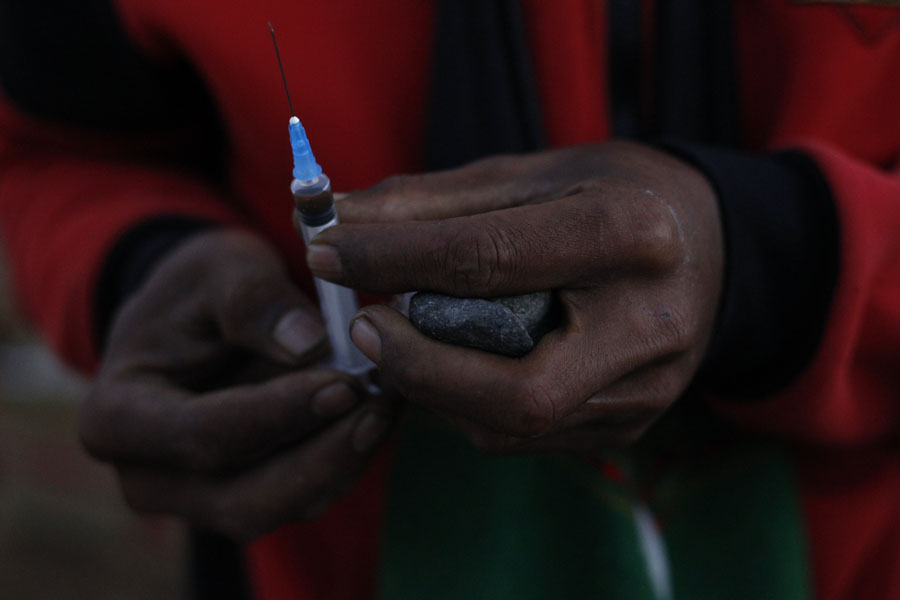
Heroin powder stored in one and a half inch vials cost about 35,000 kyats in Rangoon, according to former users in the city.
Despite millions of dollars worth of narcotics being torched every year, observers have criticized police for targeting drug addicts, recovering users and smalltime dealers over prolific drug lords.
The Myanmar National Human Rights Commission (MNHRC) reported in March that Rangoon’s notorious Insein prison was detaining about 10,000 prisoners ¬¬— 5,000 more than its maximum capacity. MNHRC last week also visited Kachin State’s Myitkyina prison and revealed that 75 percent of its 3,000 prisoners were convicted on drug-related charges, including inmates in their 70s and 80s.

Not Enough Treatment Centers
The health ministry estimated the latest figure to be more than 80,000 intravenous drug users across the country and forecasted the number to increase. Medical treatments and rehabilitation programs for drug users are promised in the 1993 law, but in reality, access to these are limited.
In the 1970s, a former superintendent of Rangoon’s Mental Health Hospital experimented with a treatment for heroin addiction that comprised opium, painkillers and sleeping pills, which was used in Burma until methadone therapy was introduced to the country in 2006, a drug that suppresses the withdrawal symptoms when addicts begin reducing their intake of heroin.
According to Dr. Nanda Myo Aung Wan, the Ministry of Health’s manager for National Drug Abuse Prevention and Control Program, Burma has 73 hospitals that have drug treatment centers. Among them, 46 hospitals, including Rangoon’s Mental Health Hospital and Thingangyun Sanpya Hospital, provide methadone therapy.
Across the country, about 80 percent of treatment-seeking drug users are heroin users, 5 percent are amphetamine users, and the rest use other forms of drugs, said the doctor.
Thingangyun Sanpya Hospital provides methadone therapy for 300 to 400 addicts on a daily basis. Rangoon’s Mental Health Hospital currently has 40 inpatients and about 600 outpatients, some of who are receiving methadone. Between 30 and 40 percent of them are 20 to 35 years old, added U Nanda Myo Aung Wan.
NGOs and other advocates for drug policy reform have said the country needs more centers for methadone treatment. Rangoon’s main source for providing the therapy – the Mental Health Hospital – is at least a two-hour drive from downtown, creating logistical and financial problems for drug users who need to reach the hospital every day.
According to the Burnet Institute, an Australia-based, non-profit organization, which has provided healthcare services in Burma since 2003, many drug users who seek treatment are stopped by a lack of methadone centers.
“There are a lot of users who want to cure their addiction,” said Dr. Soe Moe Aung, the group’s project manager for harm reduction. “But the problem is getting hospitalized because most towns have only one place where methadone treatment is available.
“The government should create more methadone centers,” he said, adding that the move would encourage drug users to seek treatment.
Decriminalizing Personal Drug Use
An addict will take dangerous risks to score, says Ko Kyaw Thu, a recovering user, as he explains the correlation between drug use and crime among addicts who cannot access treatment.
In 2007, Ko Kyaw Thu co-founded the National Drug Users Network Myanmar (NDNM) and has since been advocating the decriminalization of personal drug use. He is also consulting CCDAC about its treatment-oriented drug policy draft.
“Many people think our network is encouraging drug use when we talk about decriminalizing,” he said, insisting that the purpose of his network is to spread knowledge among users of safe drug use.
However, he marked a difference between decriminalization and legalization.
“We don’t want [the government] to legalize the drug industry,” he said. “We urge it to provide treatment for those who need help while maintaining punishment for drug dealers.
“The country loses human resources by detaining its young population in prisons. With decriminalization, the government can divert the money used for arresting and imprisoning addicts into treatment.”
Social Stigma
Not only does the fear of detention push drug users underground, says Ko Kyaw Thu, but also the social alienation linked to their habit deters them from getting the right treatment.
“People are afraid of drug users even more than bandits,” he said.
According to the Burnet Institute, drug addiction is strongly stigmatized in Rangoon, making it difficult for users to seek help.
The organization opened drop-in centers for injection drug users (IDU) in Rangoon, Mandalay, Sagaing and Pyin Oo Lwin to provide one-time use needles for IDUs, along with other services, in order to lower the risk of transmitted diseases through syringe sharing among addicts.
“If we want to open a drop-in center in Rangoon, people become afraid that drug users would come to their neighborhood and harm them,” said Dr. Soe Moe Aung.
Burnet later reduced its help in Rangoon to blood testing, counseling, and methadone referral, dropping its needles service because of protest within the community. The service continued in its other centers.
However, Dr. Soe Moe Aung stressed that drop-in centers are beneficial for drug users because they are safe resting places for users after they inject.
Stigma stretches beyond addicts and recovering addicts to people who have been imprisoned.
Ko Win Min, 48, a co-founding member of NDNM, was jailed for four years in 1994 for illegal drug use. Contributing to his distress was the discrimination he faced from some relatives.
“I even had to move out from the place I used to live [after my release],” he said.
Unable to find employment, society labeled him a “junkie” for years.
Now he counsels drug users for Burnet, acting as an important liaison between addicts, locals, and the group’s coordinators.

Patients, Not Criminals
Burnet’s country representative, Dr. Phone Myint Win, also stressed the importance of social integration for recovering users as they receive treatment.
“They could be family breadwinners,” he said. “They could be the daughters or sons who could support their families after they become clean, if they received family and social support,” he said.
The World Health Organization defines a health issue as something that damages physical, mental or social well-being. The doctor says drug addiction “devastates” all three, and so should be treated as a disease.
His colleague Dr. Soe Moe Aung agreed, saying that most people see drug addiction as a “crime.”
“Drug addiction is a chronic disease and addicts should be considered as patients,” he added.

















